The PPEC operating record from intake through daily care evidence.
Harbor is designed to organize the clinical, administrative, documentation, authorization, guardian, QA, and evidence workflows that keep a PPEC center running — with billing readiness as the downstream result of complete records.
Built for real PPEC operations
Harbor connects daily care documentation, authorizations, and billing evidence into one record — organized around the child, the day, and the center.
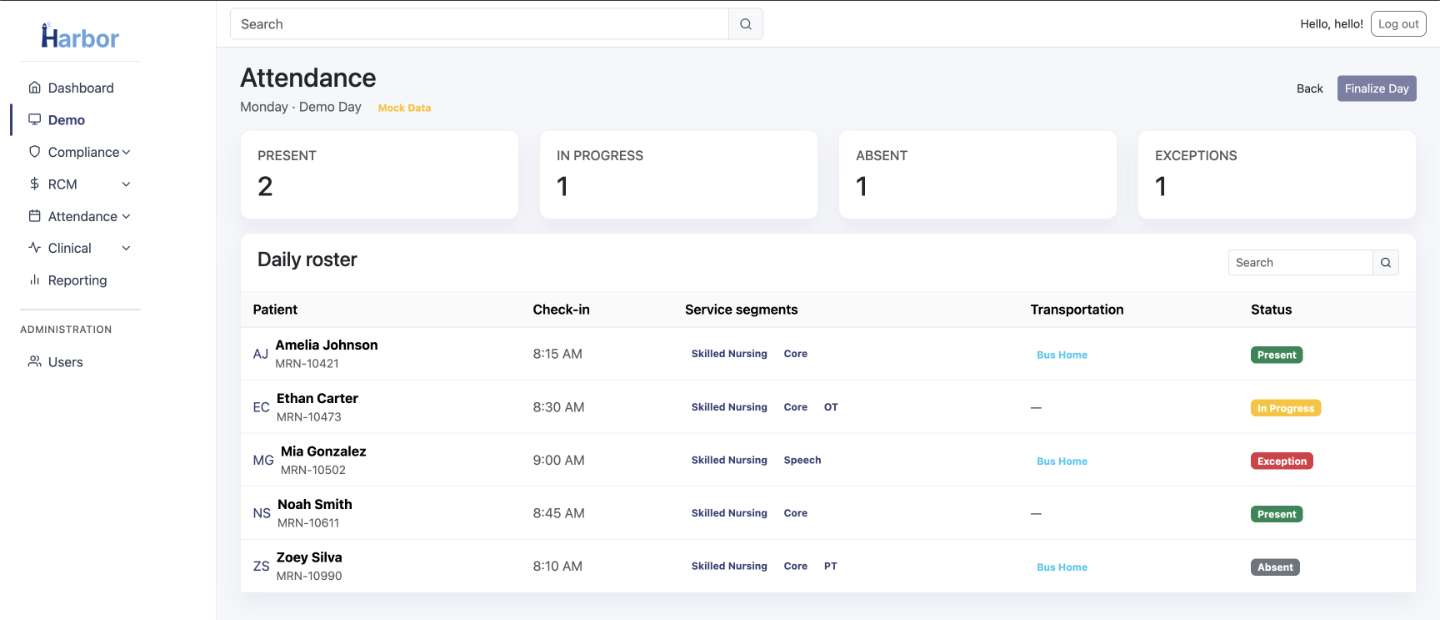
Attendance Dashboard
Daily census across nursing, therapy, and transportation — organized by child and date.
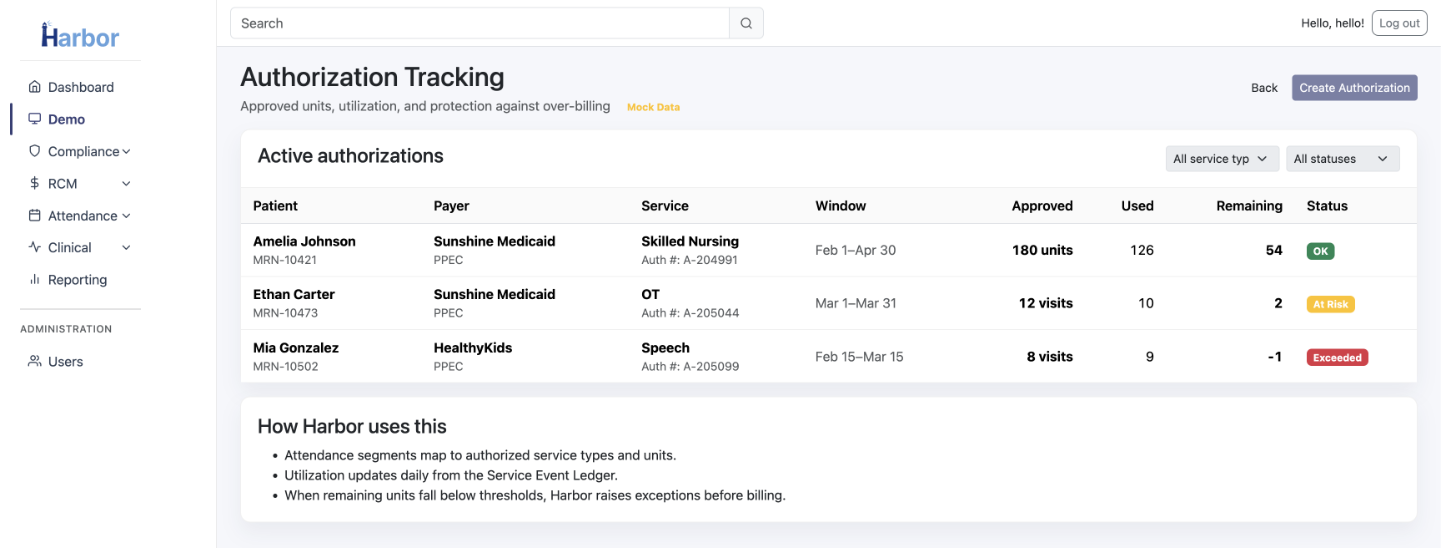
Authorization Tracking
Coverage windows, units remaining, renewal countdowns, and service component visibility.
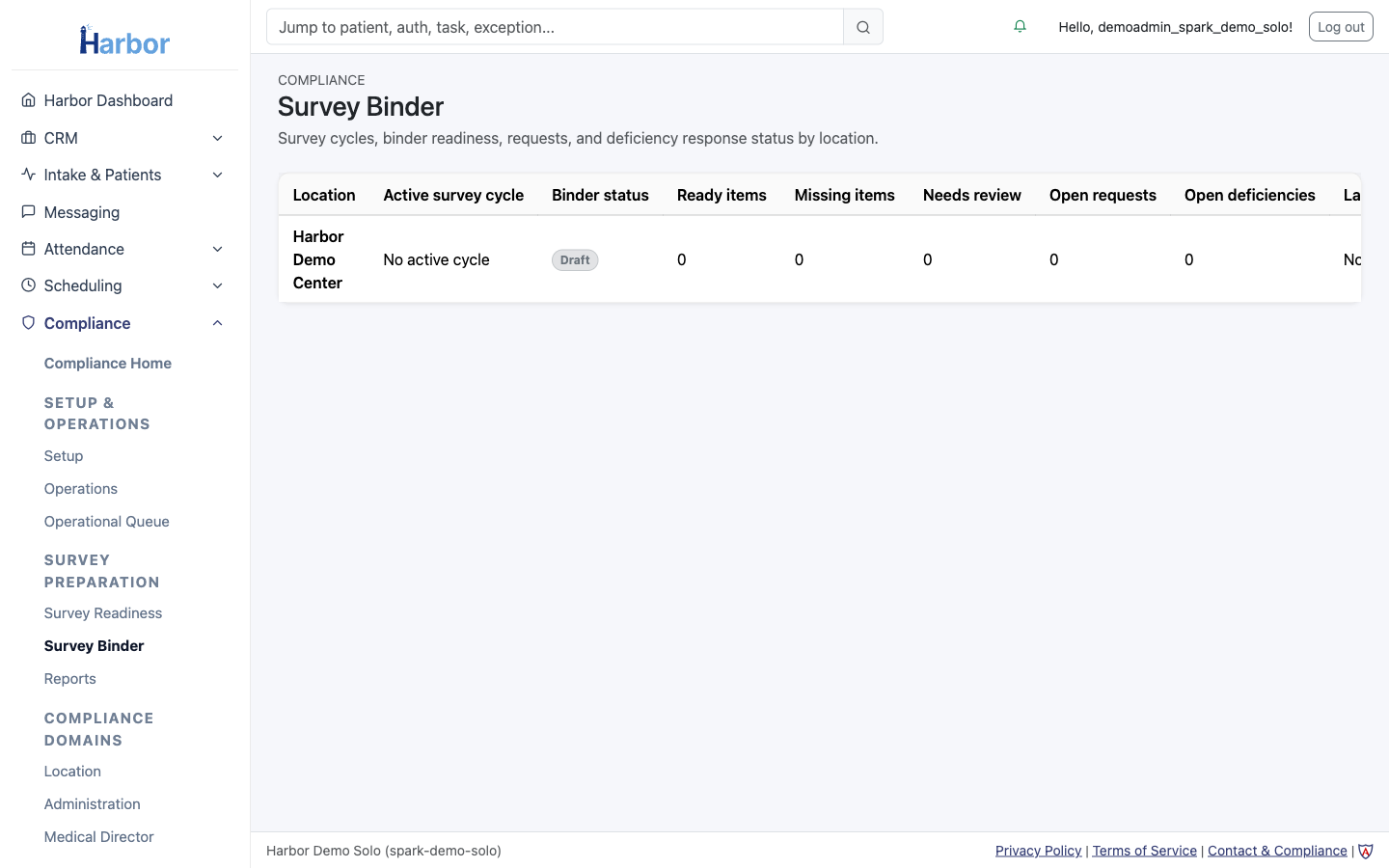
Survey / Audit Readiness
Survey binder organized and ready for review — not assembled in a panic before the surveyor arrives.
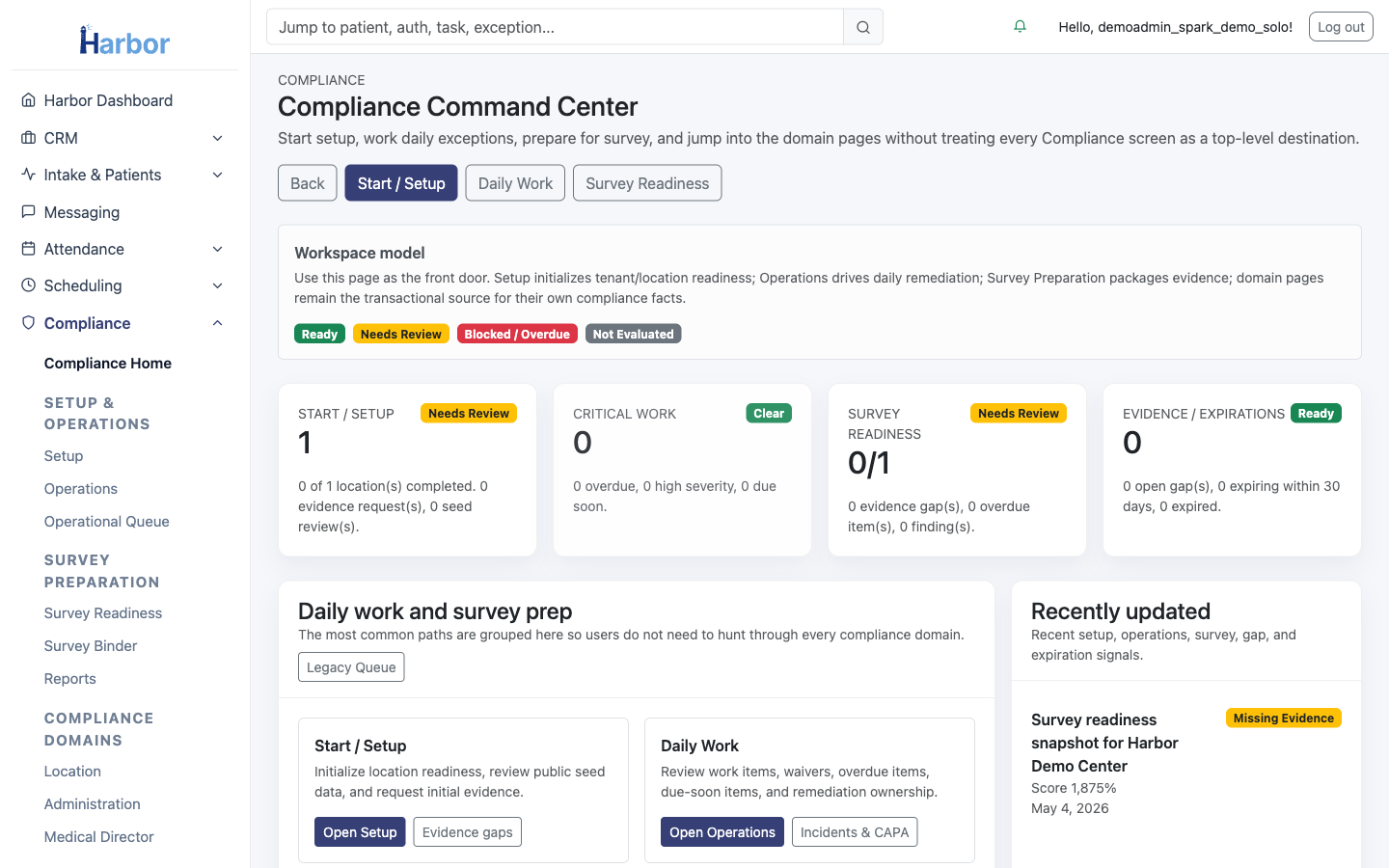
QA + Compliance Cockpit
Completeness checks, expiry monitoring, and owned work queues — before problems become gaps.
The 10 operator modules
Each module is designed to feed the next stage of the operating record — with documentation and completeness that support billing evidence downstream.
Child Clinical Profile
Care context, diagnoses, consents, plan of care, and intake documents.
Skilled Nursing Documentation
Nursing notes, visit records, and care evidence organized by child and day.
Therapy Coordination
PT, OT, speech, respiratory, developmental — documented and coordinated.
Daily Attendance + Census
Daily truth with nursing, therapy, transportation, and partial-day segments.
Authorization Tracking
Coverage windows, units, renewal countdowns, and service component limits.
Guardian / Caregiver Workflows
Communication, consents, portal access, and guardian-facing documentation.
Billing Evidence
Billing readiness as the downstream result of complete, defensible care records.
QA + Compliance Cockpit
Completeness checks, expiry monitoring, owned work queues, and audit trails.
Survey / Audit Readiness
Survey binder organization, evidence packaging, and documentation defensibility.
Integrations / Companion Mode
Start alongside existing systems before full migration — companion layer first.
Care context organized around the child.
Harbor builds the clinical picture from the ground up — intake documents, diagnoses, consents, care plans, and orders — so every subsequent workflow has the context it needs.
- Intake readiness tracking with required artifacts
- Plan of Care lifecycle and versioning
- Consents, orders, and certification tracking
Nursing documentation that supports the care record.
Harbor helps organize nursing visit records, notes, and daily care documentation — by child, by date, and by care event — so the operating record reflects what actually happened.
- Nursing visit records and care event documentation
- Documentation completeness indicators per child
- Incident reporting workflows and audit trails
Harbor organizes and tracks completeness. Licensed nurses document, sign, and make clinical determinations.
Coordinate therapies across the operating day.
PPEC centers coordinate PT, OT, speech, respiratory therapy, and other services — often with external providers. Harbor helps track what was delivered, when, and against which authorization.
- Therapy session tracking by type and provider
- Documentation completeness per therapy type
- Authorization cross-reference for therapy units
The operating truth for every center day.
Harbor captures the daily census — who attended, which nursing and therapy services were delivered, and how transportation segments fit into the day — as a first-class record that supports downstream documentation and billing evidence.
- Multi-segment attendance (nursing, therapy, transportation)
- Absences, partial-day, and transportation-only tracking
- Census visibility for capacity and operational planning

Authorization visibility across the operating day.
Harbor keeps coverage windows, service components, units, and renewal timelines present and visible — so centers are not discovering authorization gaps during billing review.
- Coverage windows, service components, and unit limits
- Renewal countdown and expiry visibility
- Transportation and therapy authorization cross-reference
Keep families connected to the operating record.
Guardians and caregivers are part of PPEC care. Harbor organizes consents, communication, and guardian-facing documentation so families stay informed and the center maintains a complete record.
- Guardian consent tracking and document history
- Family portal access and communication
- Guardian-facing daily summary and attendance visibility
Billing Evidence
Billing readiness is the downstream result of a complete, documented operating record — not a separate pipeline that runs in parallel.
Documentation completeness review
Harbor helps surface documentation gaps before billing review — so the team is reviewing complete work, not hunting for missing records.
Evidence traceability
Trace billing evidence back to the child, day, authorization, and care documentation that supports it.
Claim readiness indicators
Harbor helps prepare the operating record for billing review — surfacing gaps and completeness status before handoff to the billing team.
Completeness by design — not by scramble.
Harbor surfaces documentation gaps, expiry warnings, and completeness issues as owned work items — so QA teams can review and resolve before they become problems.
- Documentation completeness checks and expiry monitoring
- Owned work queues with due dates and role assignments
- Unified audit trail across modules and actions
See Compliance for full details on documentation controls and auditability.

Survey binder — organized, not assembled.
Harbor helps organize the documentation that surveyors and auditors ask for — so the center can respond quickly and defensibly without a last-minute scramble.
- Survey binder organization and evidence packaging
- Audit defensibility through traceable, complete records
- Readiness status visible before surveys happen

Integrations / Companion Mode
Harbor is designed to start alongside existing systems — not require a complete replacement on day one.
Companion layer first
Harbor can operate alongside existing EHR, billing, or spreadsheet workflows — adding the operating record layer without forcing immediate migration.
Staged rollout
Start with census and documentation, add authorization tracking, then expand to QA and billing evidence — at the pace that works for the center.
External provider coordination
Coordinate with external therapy providers, transportation vendors, and billing teams without requiring everyone to be in one system on day one.
Want to walk through the operating record?
Tell us about your center workflow and we'll map where Harbor can begin safely.